BLADDER CANCER
Treatments
Contact Us
If you would like to make an appointment please get a referral from your doctor first. We can then work with you to find the appropriate treatment plan.
Bladder Cancer
Bladder cancer is responsible for approximately 3% of all malignancies diagnosed in Australia each year. Bladder cancer is more common in men than women and typically affects people over 60 years of age.
The most common sign of bladder cancer is haematuria (blood in the urine), which is usually painless and may appear only from time to time over a period of months. It is essential to have full investigation if you notice haematuria.
If a bladder tumour blocks a ureter (one of the two tubes that pass urine out of the kidneys and into the bladder), patients may experience pain in the side of the body between the ribs and the top of the hip.
Diagnosis
If there is blood in the urine your doctor will need to conduct some physical examinations in order to formulate an accurate diagnosis.
Cystoscopy
During a cystoscopy a thin flexible tube with a light and a camera lens is inserted into the urethra and up into the bladder, allowing the doctor to look at the inner lining of the bladder and check for any abnormalities or suspicious looking tissue. The doctor may also take a biopsy that can be examined more closely in a laboratory allowing an accurate diagnosis to be made.
CT Intravenous Pyelogram or CT IVP
A special dye is injected your arm that travels through the bloodstream to the urinary tract, which in turn is then picked up through a CT scan. This process allows a doctor to see if there are any abnormalities in the bladder or urinary tract.
Urine Cytology
The urine may contain cancer cells and Urine Cytology tests search for such cells through the pathology lab.
Treatments
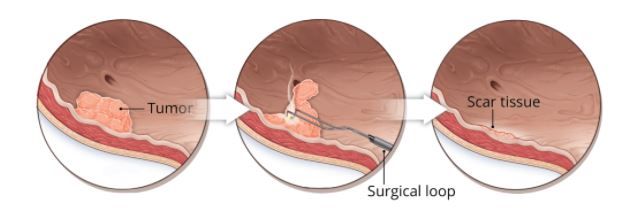
The vast majority of bladder cancers do not penetrate deep into the bladder wall and are able to be removed and cured through treatment with a cystoscope. This is called Trans Urethral Resection of Bladder Tumour – TURBT.
After removal the area is coagulated to control bleeding and kill any remaining cancer cells. Such tumours may recur and patients will be entered on a Surveillance Program to inspect the bladder regularly over a period at least 5 years.
If the tumours recur it may be required to treat with Chemotherapy agents such as BCG or Mitomycin. Mr Donnellan will discuss this if required.
Bladder cancers that have grown deep into the bladder wall or into surrounding tissue usually require major open surgical therapy to remove the bladder. This is called Radical Cystectomy.
For women, a standard form of surgery is a Radical Cystectomy, which involves cutting away the entire bladder and associated tissues, with Pelvic Lymphadenectomy (removal of the lymph nodes within the hip cavity). Radical cystectomy in women includes removal of the uterus, Fallopian tubes, ovaries, anterior vaginal wall (the front of the birth canal), and urethra.
In men, a common surgical procedure is called a Cysto-Prostatectomy, which involves the removal of the bladder and prostate, with Pelvic Lymphadenectomy.
Urinary Diversion
If the bladder is removed, an alternative forms of urine drainage is needed. The most common diversion is called an Ileal Conduit – this involves taking a piece of bowel and forming a ‘pipe’ that is inserted where the bladder once was. The conduit then carries the urine from the ureters out onto the skin of the abdomen where the conduit ends in a Stoma – a small opening. Urine is then emptied into a plastic bag attached to the skin, where it can be emptied at various intervals.
Other forms of diversion involve the formation of an internal pouch made out of part of the bowel. The pouch has an inbuilt valve so that urine collects inside and does not leak through the Stoma. When it needs emptying, a small plastic tube called a Catheter can be passed through the stoma and the valve allowing urine to flow out. This is a major piece of surgery and requires much planning and recuperation time.
These types of surgery are very significant and often require 2 surgical teams – one to remove the bladder and associated organs and lymph nodes, and one to form the new Urinary Diversion.